What Every Parent Should Know Before Leaving Medicine Out
Why Child-Resistant Caps Fail (& the 5 Medicine Habits That Actually Protect Your Child)
In more than 50% of cases where children accessed prescription pills, an adult had already removed them from child-resistant packaging, according to CDC poisoning surveillance data. [1] This guide reveals the 5 moments medicine becomes dangerous and the prevention habits that work when caps fail.
It’s strange how easily medicines lose their danger in our minds.
They sit on bedside tables, inside handbags, next to sinks, tucked into fridge doors. We use them to heal, so we start to feel they’re safe.
But for your child, especially a curious one, medicine isn’t “treatment.” It’s just something to taste, open, or copy. And that’s where the risk begins.
You’re being careful — I know you are. But when I studied recent pediatric poisoning data, one pattern kept emerging: medicines are the leading cause of poisoning in young children, and the highest-risk years are ages one to three — when mobility and curiosity surge faster than adults can adjust the home. [2][3][4]
Here’s what caught my attention: almost every medicine can become harmful if taken the wrong way. Too much. Too often. Taken by the wrong child. Even vitamins and herbal products fall into this category. [2][3][5]
The label might say “over-the-counter” or “natural,” but that doesn’t make it safe in a child’s hands.
Why This Guide Is Different From Generic Medication Safety Lists
Research-backed from poison control centers: Every recommendation comes from emergency department data, pediatric toxicology studies, and medication safety research (2011-2024).
Islamic perspective integrated: This isn’t just about locking cabinets — it’s about honoring the amanah (sacred trust) of protecting vulnerable children through both practical habits and spiritual awareness.
Immediate action plan included: You’ll get a free Medicine Safety Home Audit to walk through your entire home in 15 minutes and catch every hidden medicine risk — not just information, but a checklist that works.
The Real Reason Child-Resistant Caps Don’t Work
Here’s something most parents don’t realize: “child-resistant” does not mean “child-proof.”
Children still get in. If a child has enough time and access, caps and latches can fail. But there’s something even more important that the CDC data revealed: in more than half of pediatric poisoning cases involving prescription medications, an adult had already removed the pills from the child-resistant container. [1]
Let me say that again.
The safety feature worked. But we bypassed it.
Pill organizers. Pills set on the counter “just for a moment.” Tablets in a handbag. Medicine moved to an easy-open bottle because the original cap was too difficult.
That’s why medicine safety isn’t only about bottles in locked cabinets. It’s about the five critical moments when medicine becomes accessible.
The 5 Critical Moments When Medicine Becomes Dangerous
Moment 1: During Use (When the Bottle Is Already Out)
Many poisoning cases don’t come from long-term storage failures. They happen during use, when the bottle is already out and your attention shifts for just a moment. [6]
A phone rings. A sibling needs help. The doorbell sounds. You set the open bottle down “just for a second.”
That’s the moment.
Here’s what works: Put the medicine back in its locked storage immediately after use — not “in a minute,” not after you finish the task. [2][6][7] The moment you’re done dosing, the bottle goes back up high and locked.
Moment 2: Pill Organizers and Daily Dose Containers
I know pill organizers make life easier, especially when multiple family members take medications. But here’s what poison control data shows: these containers bypass every child-resistant feature of the original packaging.
If you use pill organizers, they need to be stored with the same care as prescription bottles — locked, high, out of sight. [2][6]
Moment 3: Handbags and Diaper Bags
This is one of the most overlooked risks in medicine safety, and I want you to hear this clearly: handbags often contain medicines, hand sanitizer, vitamins, supplements, and other substances children shouldn’t swallow. [2]
Because a bag belongs to an adult, it often escapes the childproofing mindset entirely. It shouldn’t.
Your purse, your partner’s bag, visiting relatives’ handbags — they all need to stay off the floor and out of reach.
Moment 4: When Routines Change (Visitors, Travel, Moving)
Unfamiliar environments often mean medicines are left in accessible places without anyone noticing quickly enough. [2] The safest assumption is that any change in routine requires extra attention.
When grandparents visit, when you travel, when you move house — these are high-risk windows. Before visitors arrive, have a conversation: “We keep all medicines locked up. Can you please keep yours in your room on a high shelf or in your locked suitcase?”
Moment 5: Bedside Tables and Bathroom Counters
I understand why medicine ends up on bedside tables. Late-night doses. Morning routines. Chronic conditions requiring easy access.
But studies on parental perceptions show that adults often overestimate what’s “high enough” or “safe enough,” especially once a medicine becomes part of the familiar routine. [8]
If medicine must be accessible for adult use, it needs to be in a locked box on that bedside table — not just sitting there.
I know this is a lot to remember when you’re managing daily routines, medications for multiple family members, and everything else. That’s why I’ve created a free Medicine Safety Home Audit — a room-by-room checklist that walks you through your entire home in 15 minutes. Keep reading to download it at the end — it’s designed to help you catch every hidden risk without relying on memory alone.
The Small Habits That Prevent Big Harm
Beyond storage, there are habits around medicine use that quietly reduce risk.
Slow down enough to read labels carefully. Check the dose. Confirm you’re giving the right medicine to the right child at the right time. [2][9][10]
That might sound obvious, but when there are multiple children, different prescriptions, or shared caregiving, mistakes happen more easily than expected. Research on medication safety shows that dosing errors are a common reason for pediatric poisoning incidents. [3][9]
That’s why some families keep a simple written record near the medicine — just time and dose — especially when more than one adult is involved. Not because they’re overly cautious, but because memory isn’t reliable when routines shift.
Keep Medicines in Their Original Containers
This matters more than it seems. Once something is poured into a different bottle or container, its identity disappears. [2][7]
To a child, it may look like juice, candy, or something familiar. To an adult in an emergency, it becomes harder to identify what was taken.
Even substances people don’t immediately think of as “medicine” — like essential oils, nicotine replacement products, or concentrated supplements — can be harmful in children. [2][5]
The Medicines That Require Extra Care
Some medicines are more dangerous than others, even in small amounts. These categories require particular vigilance: antidepressants, heart medications, diabetes medicines, strong painkillers, ADHD medications, iron tablets, and sleeping tablets. [2][3][5]
Many of these affect vital systems in the body and can cause serious harm quickly if taken incorrectly.
What Children See Matters
If your child watches you take medicine regularly, especially if it’s described casually or sweetly — “this will make me feel better” or “just my little tablets” — they may try to imitate that behavior.
Instead of calling medicine “candy” or “lollies,” use proper names. [2] This small shift in language helps children understand that medicine is different from food.
If a Child May Have Taken Medicine
Stay calm. Gather the container or packaging. Seek immediate professional advice rather than waiting for symptoms to appear. [2][7]
Contact your local poison control center immediately — don’t wait for symptoms.
If your child is collapsing, seizing, hard to wake, or struggling to breathe, call emergency medical services right away.
Because symptoms can be delayed, and guessing what to do can cause more harm than the exposure itself.
The Islamic Framework for Medicine Safety
When I reflect on the verse where Allah says, “O you who believe, protect yourselves and your families from a Fire...” [11], I think about how protection includes physical safety and daily decisions that prevent harm before it reaches those who cannot prevent it themselves.
A child does not understand risk the way you do. Their safety depends on you thinking ahead on their behalf.
Another verse reminds us: “And do not kill yourselves [or one another]. Indeed, Allah is ever Merciful to you.” [12] Part of that mercy is guidance — warning us away from avoidable harm.
The Prophet ﷺ said, “A man is a guardian over his family and is responsible for them.” [13] That responsibility doesn’t only show up in big moments. It shows up in quiet habits: closing a cap properly, putting a bottle away, checking a label again even when tired.
He also said, “The believer is not stung from the same hole twice.” [14] There’s wisdom in that. When we learn where harm can come from, we adjust. We don’t repeat the same exposure.
And the hadith reminds us: “Actions are judged by intentions.” [15] A parent who builds careful routines around medicines — even when no incident has happened — is acting with foresight, not fear. That intention carries weight, even in something as ordinary as locking a cupboard.
Prevention Is Built in Ordinary Moments
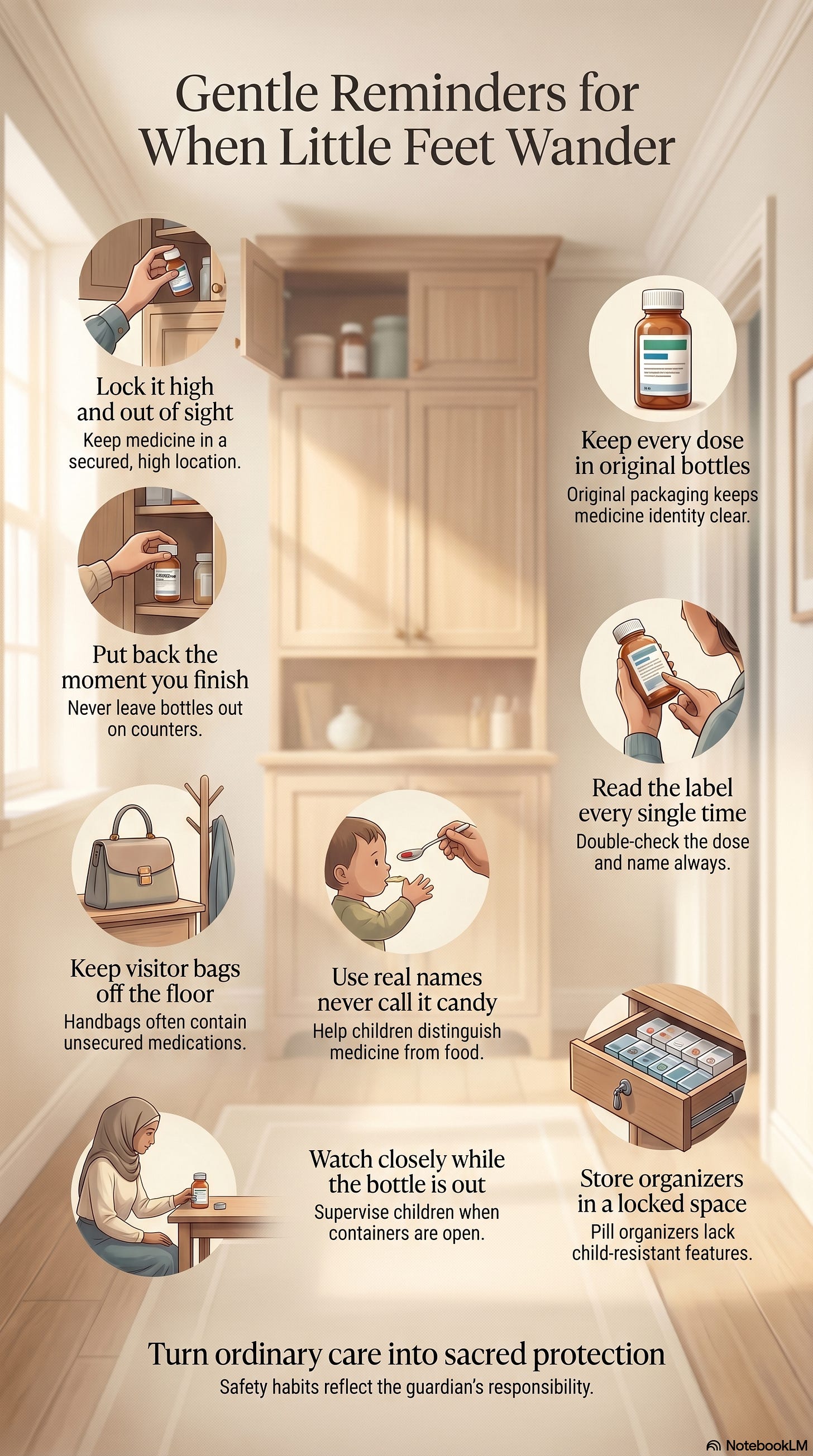
So prevention is not one dramatic action. It’s a pattern:
Lock it away — high, out of sight, in locked storage.
Put it back immediately — not “in a minute,” but the moment you’re done.
Keep it in original packaging — so identity is never lost.
Check before giving — read labels, confirm dose, verify the right child.
Watch during use — supervision matters most when medicine is already out.
Stay alert when routines change — visitors, travel, moves require extra attention.
None of it feels heroic. But together, it creates a safer space.
Because in the end, safety isn’t built in emergencies. It’s built in ordinary days, repeated choices, and the moments no one notices.
If you’ve read this far, you’re the kind of parent who takes medicine safety seriously — not as paranoia, but as protective love. That tells me something beautiful about you.
Your Medicine Safety Home Audit
Inside the Medicine Safety Home Audit (one comprehensive PDF, 3 pages):
Page 1: Room-by-Room Medicine Storage Checklist — A walk-through audit for your bathroom, bedroom, kitchen, handbags, and visitors’ spaces with yes/no questions and immediate action items — designed so you can complete your entire home in 15 minutes and know exactly what to secure.
Page 2: Emergency Medicine Poisoning Response Card — What to do (and what NOT to do) if you suspect your child has taken medicine, including poison center contact guidance, signs requiring immediate emergency care, and space for your local numbers — designed as a laminated card for your fridge or first aid kit.
Page 3: Medicine Safety Du’as for Daily Routines — Morning protection prayers, du’a when giving medicine to a child, and evening safety prayers (Arabic, transliteration, English) — organized by your daily rhythm so these become habits, not afterthoughts.
This isn’t just a PDF to download and forget. It’s a tool designed to help you protect your family in the moments when medicine actually becomes dangerous.
This Medicine Safety Home Audit is what every GrowDeen subscriber receives with each article. We cover the full journey of raising Muslim children — from safety and health to character development and daily Islamic routines — all backed by research and rooted in wisdom.
If you’re a Muslim parent who wants both evidence-based guidance AND Islamic perspective, subscribe for free so future resources arrive in your inbox before you need them — whether that’s navigating fevers, teaching Salah habits, or understanding developmental milestones through an Islamic lens.
You’ll receive one article when it’s ready — no daily emails, no clutter, just guidance when there’s something worth sharing.
May Allah place barakah in your effort, accept your intention, and make the care you give more protective, more merciful, and more rewarded than it feels in the moment.
Share This With Someone Who Needs It
Think of one person right now: a parent with multiple medications in the house, a grandparent who visits regularly with pills in their handbag, a friend whose toddler just learned to climb and open bottles, or a family member who uses a pill organizer on the kitchen counter.
This article could prevent a poisoning. Share it with them today — not because you’re being preachy, but because you care. Sometimes the most loving thing we can do is pass along knowledge that prevents tragedy.
References
[1] Centers for Disease Control and Prevention (CDC). Medication safety surveillance data on pediatric exposures to prescription medications removed from child-resistant packaging.
https://www.cdc.gov/
[2] Huynh, A., Cairns, R., Brown, J.A., Lynch, A-M., Robinson, J., Wylie, C., Buckley, N.A., & Dawson, A.H. (2018). Patterns of poisoning exposure at different ages. Medical Journal of Australia, 209(2), 74-79.
[3] Lee, V.R., Connolly, M., & Calello, D.P. (2017). Pediatric poisoning by ingestion. Pediatric Annals, 46(12), e443-448.
[4] Schmertmann, M., Williamson, A., Black, D., & Wilson, L. (2013). Risk factors for unintentional poisoning in children aged 1–3 years. BMC Pediatrics, 13, 88.
[5] Ozdemir, R., Bayrakci, B., Tekşam, O., Yalçin, B., & Kale, G. (2012). Childhood poisoning patterns. Turkish Journal of Pediatrics, 54(3), 251-259.
[6] Kendrick, D., Majsak-Newman, G., Benford, P., Coupland, C., Timblin, C., Hayes, M., Goodenough, T., Hawkins, A., & Reading, R. (2017). Poison prevention practices and medically attended poisoning in young children. Injury Prevention, 23(2), 93-101.
[7] NSW Poisons Information Centre. Prevention guidance for poisoning in the home.
https://www.poisonsinfo.nsw.gov.au/
[8] Rosenberg, M., Wood, L., Leeds, M., & Wicks, S. (2011). Parental perceptions and childhood poisoning risk. Health Promotion Journal of Australia, 22(3), 217-222.
[9] The Royal Children’s Hospital Melbourne (RCH). Medicines for children and medicine reactions.
https://www.rch.org.au/
[10] The Sydney Children’s Hospitals Network (SCHN). Medication safety for children.
https://www.schn.health.nsw.gov.au/
[11] Quran, Surah At-Tahrim 66:6
[12] Quran, Surah An-Nisa 4:29
[13] Sahih al-Bukhari 7138
[14] Sahih al-Bukhari 6133; Sahih Muslim 2998
[15] Sahih al-Bukhari 1; Sahih Muslim 1907