The Everyday Products That Poison 50,000 Children a Year
If You Have a Toddler, Read This Before Cleanup Time
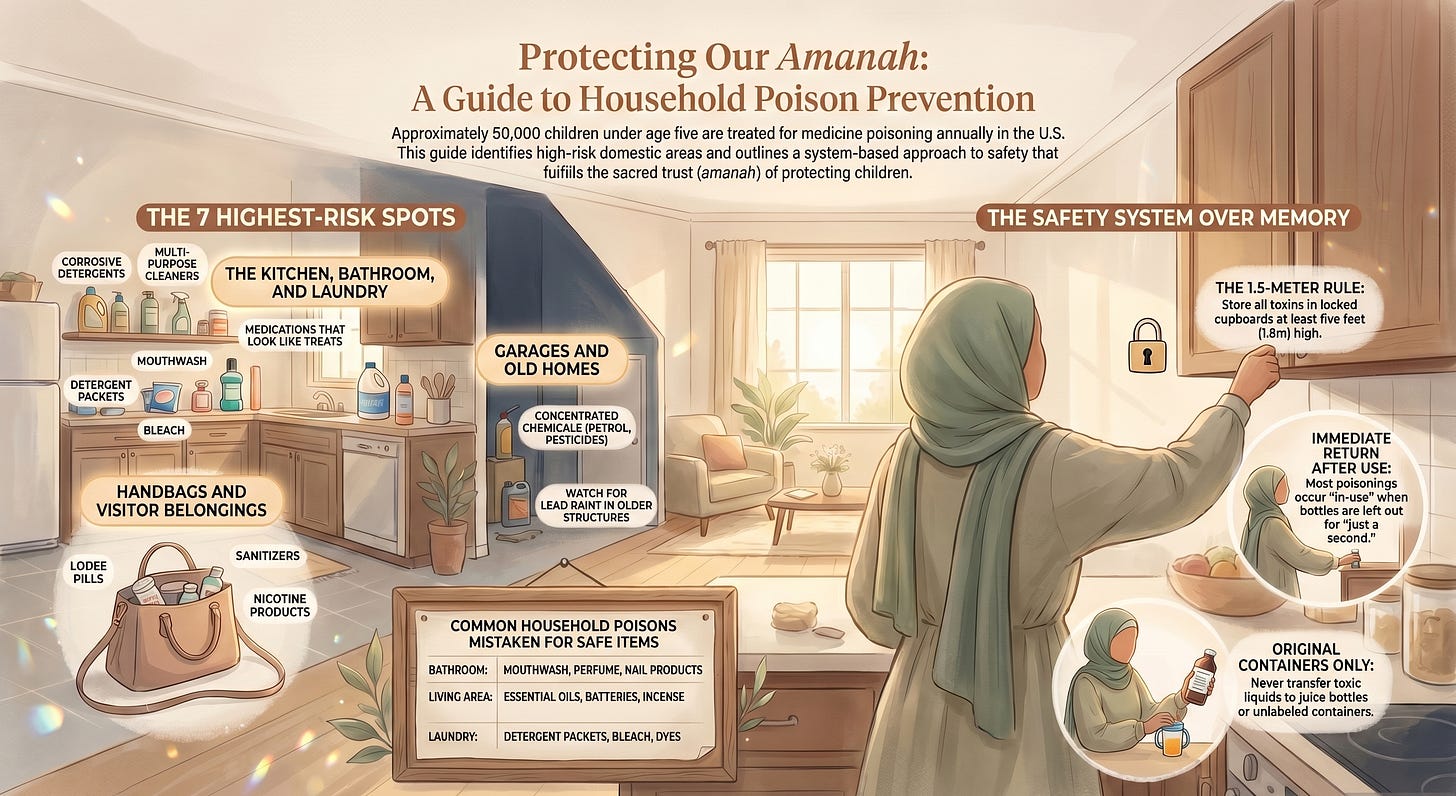
U.S. emergency departments treat approximately 50,000 children under age five each year for medicine poisoning alone and most exposures happen in ordinary moments when products are in use, not just in storage. [1] This guide shows you the 7 highest-risk spots in your home and the prevention habits that actually work.
A bottle left on a low counter. Tablets in a handbag. Detergent moved for “just a second.” A child who learned to climb last week and can now open what looked impossible yesterday.
This is how poisoning usually begins at home. Not with rare chemicals in unusual places, but with everyday products in ordinary rooms. [2][3][4]
You’re being careful — I know you are. But here’s what caught my attention when I studied recent poison center data: the highest-risk years aren’t when children are newborns. They’re when mobility and curiosity surge faster than adults adjust the home. [2][3][5]
Children under five face the greatest poisoning risk, and the danger peaks in the toddler years when they’re learning to climb, twist lids, and explore in ways you didn’t expect last month. [2][3][4][5]
Here’s why:
Every new skill brings new poisoning risks. Research on parental perceptions shows that adults often overestimate what’s “high enough” or “safe enough” — especially once a product is put back in a familiar spot. [6]
That’s one reason poisoning prevention depends less on your memory and more on systems.
Why This Guide Is Different From Generic Safety Lists
Current research from pediatric poison centers: Every recommendation is backed by emergency department data, poison control analyses, and prevention studies from 2013-2024.
Islamic framework integrated: This isn’t just a list of what to lock up — it’s about fulfilling the amanah (sacred trust) of protecting vulnerable children through both practical systems and spiritual awareness.
Room-by-room action plan included: You’ll get a free Poison Prevention Home Audit Kit to walk through your entire home in 20 minutes — not just information, but a checklist you’ll actually use.
The Storage System That Matters More Than Your Memory
The most important prevention system is storage. Here’s what works:
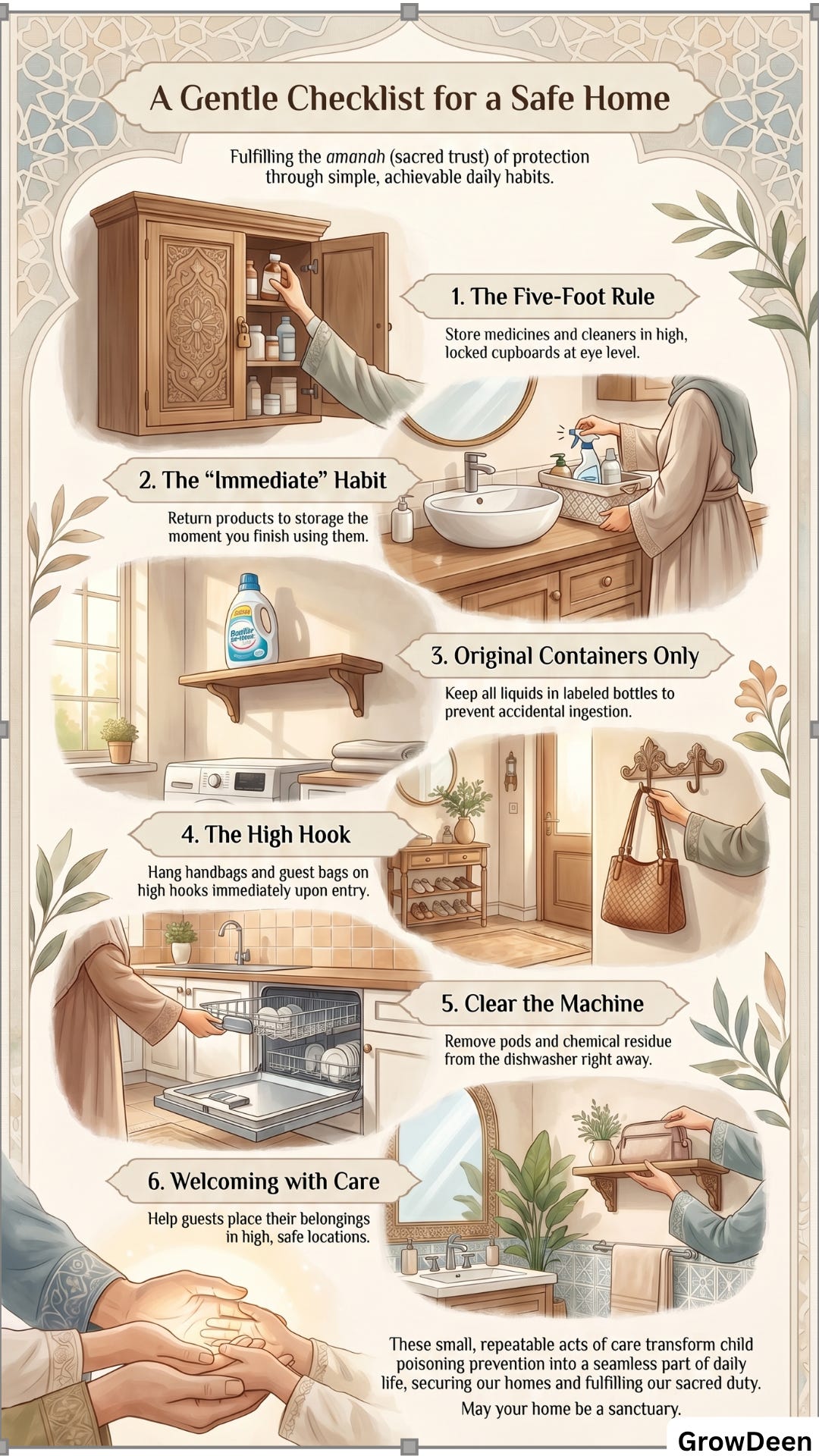
Keep poisons up high, out of sight, and in locked cupboards — ideally around 1.5 meters (5 feet) high with child-resistant locks. [2][7][8] The American Academy of Pediatrics uses broader language but emphasizes the same principle: medicines, cleaning products, paints, pesticides, detergent packets, and other toxic products should be stored in locked cabinets or containers, completely out of children’s sight and reach. [1]
But here’s something critical that most parents don’t realize: “child-resistant” does not mean “child-proof.”
Children still get in. If a child has enough time and access, caps and latches can fail. That’s why the next habit matters so much.
The “In Use” Moments When Most Poisonings Happen
Poisons should go back to their locked storage immediately after use — not “in a minute.” [2][7][8]
Many poisoning incidents don’t happen during long-term storage. They happen during use. A cleaning spray on the floor while you wipe a surface. A medicine bottle open on the table. Drain cleaner left by the sink. Weed killer out during yard work.
When I reviewed poison center case reports, this pattern kept emerging: supervision matters most in those live moments when the product is already out and a child is nearby.
Why Original Containers Aren’t Negotiable
Household poisons must stay in their original containers. [2][7][8]
A toxic liquid in a juice bottle or soft-drink container is one of the clearest ways to accidentally make poison look safe. The WHO’s poison-control guidance stresses the importance of correct identification, proper labeling, and access to product information in both poisoning prevention and emergency management. [9]
I can’t stress this enough: even if you think you’ll remember what’s in that unlabeled spray bottle, your child won’t know. And neither will emergency responders if something goes wrong.
Medicine Deserves a Stronger Warning Than Most Families Give It
Here’s what stopped me when I studied the data: medicines are the most common cause of poisoning in young children, and almost all medicines can be poisonous if used improperly — including vitamins and herbal remedies. [2][3][4][8]
The AAP reports that around 50,000 children under five in the United States end up in emergency departments each year after getting into medicines. [1] And CDC data shows that more than half the time, children accessed prescription pills that an adult had already removed from the child-resistant container.
So medicine safety isn’t only about bottles in a locked cabinet. It’s also about pill organizers, handbags, bedside tables, counters, and the pills you set down “just for a moment.”
Handbags are one of the most overlooked risks. They often contain medicines, hand sanitizer, makeup, sunscreen, nicotine products, and other substances children shouldn’t swallow. [2] Because a bag belongs to an adult, it escapes the childproofing mindset entirely.
It shouldn’t.
The 7 Highest-Risk Spots in Your Home
I know remembering every dangerous product in every room feels overwhelming, especially when you’re managing toddlers and daily routines. That’s why I’ve created a free Poison Prevention Home Audit Kit — a room-by-room checklist with photos and action steps. Keep reading to download it at the end of this article — it’s designed to help you walk through your home in 20 minutes and catch every hidden risk.
1. Bathrooms: More Than Just Medicines
Bathrooms hold cleaners, mouthwash, perfume, aftershave, hand sanitizer, nail products, and medicines. [2][4][10] Some of these carry high alcohol content or corrosive ingredients that burn on contact.
2. Bedrooms and Family Areas: The Quiet Risks
Air fresheners, alcohol, glues, paints, incense, mothballs, cigarettes, bubble solution, and essential oils. [2][4][10][11]
The mention of essential oils matters more than you might think. Poison center analyses have found significant exposures in children, especially with eucalyptus and other concentrated oils. [10]
3. Kitchens and Laundry: Where Products Look Ordinary
Dishwashing and laundry detergents, disinfectants, bleaches, drain cleaners, dyes, sprays, floor cleaners, rat poisons, and hand sanitizer. [2][4][8]
Dishwasher detergent needs special attention: these products are corrosive, can burn the mouth and throat, and may leave dangerous residue inside the machine even after the cycle finishes. [2]
Recent pediatric injury reports highlight cleaning products — especially detergent packets and spray bottles — as major causes of emergency visits in young children. [12]
4. Garages and Sheds: The Concentrated Dangers
Petrol, kerosene, pesticides, herbicides, paint thinners, glues, solvents, car-care chemicals, fertilizers, and epoxies. [2][4][7][8]
A locked garage is good. A locked garage plus locked cupboards inside is better. The more barriers between your child and the poison, the safer they are.
5. Handbags and Diaper Bags
Already mentioned, but worth repeating: handbags and diaper bags bypass every childproofing system if they’re left on the floor or low furniture.
6. Visitors’ Belongings
Grandparents’ pill organizers. Friends’ purses. Overnight guests’ toiletry bags. These often sit in easy-to-reach spots because visitors don’t think like parents.
7. Old Homes: The Lead Paint Risk
Older homes and furniture may contain lead-based paint, which poisons children if flakes or dust are swallowed or inhaled. The WHO continues to warn that lead exposure harms children’s developing brains and remains a major global health problem. [13]
What to Do If You Suspect Poisoning
If you think your child has swallowed, inhaled, touched, or gotten into something poisonous:
Contact your local poison center or poison information service immediately — don’t wait for symptoms to appear. [2]
If your child is collapsing, seizing, hard to wake, or struggling to breathe, call emergency medical services right away.
The WHO describes poison centers as specialized services that provide expert advice on diagnosis and management of poisoning and help guide urgent response. [9]
What NOT to Do
Don’t guess treatment. Don’t force vomiting. Don’t wait for symptoms if a dangerous exposure is suspected.
Some poisons burn more if vomited. Some need dilution. Some need urgent emergency care. Guessing is where harm multiplies.
The Islamic Framework for Poisoning Prevention
When I reflect on the verse where Allah says, “And let those fear [Allah] who, if they left behind weak offspring, would be concerned for them” [14], I think about how household safety sits naturally inside that concern for vulnerable children.
Another verse reminds us: “Do not pursue that of which you have no knowledge.” [15] In a poisoning emergency, that means not improvising treatment from hearsay, not relying on home myths, and not assuming “it was only a little.”
Allah also says, “And cooperate in righteousness and piety.” [16] Poison prevention in a home is often cooperative work. One adult stores medicines properly, another reminds visitors to keep handbags up high, older siblings learn not to leave products around.
The Prophet ﷺ said, “Each of you is a shepherd, and each of you is responsible for his flock.” [17] A child’s safety around medicines, chemicals, and cleaning products is part of that shepherding.
He also said, “There should be neither harming nor reciprocating harm.” [18] If an avoidable harm is already known, the responsible thing is to remove it before it reaches the child.
And the Prophet ﷺ said, “Allah is gentle and loves gentleness in all matters.” [19] Gentleness here looks like discipline: putting the bottle away immediately, relocking the cupboard, checking the floor after using a product, not becoming careless just because something has sat there “for years.”
Prevention Is Repetitive And It Works
Household poisoning prevention isn’t glamorous. It’s repetitive, sometimes inconvenient, and easy to postpone.
But it works.
Locked cupboards. Original containers. Immediate return to storage. Medicines and handbags out of reach. Extra care during moves, holidays, and visits when routines change.
These are small acts. Yet they’re exactly the acts that keep ordinary homes from becoming dangerous ones.
If you’ve read this far, you’re the kind of parent who takes safety seriously — not as paranoia, but as protective love. That tells me something beautiful about you.
Your Poison Prevention Home Audit Kit
Inside the Poison Prevention Home Audit Kit (one comprehensive PDF, 3 pages):
Page 1: Room-by-Room Poison Safety Checklist — A walk-through audit for your bathroom, kitchen, laundry, bedrooms, garage, and outdoor spaces with yes/no questions and action items — designed so you can complete your entire home in 20 minutes and know exactly what to fix.
Page 2: Emergency Poisoning Response Card — What to do (and what NOT to do) if poisoning is suspected, including poison center contact guidance, signs that require immediate emergency care, and a space to write your local emergency numbers — designed like a laminated card you can keep on your fridge.
Page 3: Child Safety Du’as for Daily Routines — Morning protection prayers, du’a before using household products, and evening safety prayers (Arabic, transliteration, English) — organized by your daily rhythm so you can make them a habit.
This isn’t just a PDF to download and forget. It’s a tool designed to help you protect your family in the spaces where poisoning actually happens.
This Poison Prevention Home Audit Kit is what every GrowDeen subscriber receives with each article. We cover the full journey of raising Muslim children — from safety and health to character development and daily Islamic routines — all backed by research and rooted in wisdom.
If you’re a Muslim parent who wants both evidence-based guidance AND Islamic perspective, subscribe for free so future resources arrive in your inbox before you need them, whether that’s managing fevers, teaching Salah habits, or understanding developmental milestones through an Islamic lens.
You’ll receive one article when it’s ready — no daily emails, no clutter, just guidance when there’s something worth sharing.
May Allah place barakah in your effort, accept your intention, and make the care you give more protective, more merciful, and more rewarded than it feels in the moment.
Share This With Someone Who Needs It
Think of one person right now: a new mother with a curious toddler, a friend whose child just started climbing, a grandparent who keeps medicines in an unlocked bathroom cabinet, or a family member whose garage is full of unlocked chemicals.
This article could prevent a poisoning. Share it with them today — not because you’re being preachy, but because you care. Sometimes the most loving thing we can do is pass along knowledge that prevents tragedy.
References
[1] American Academy of Pediatrics (AAP). Poison Prevention & Treatment Tips; Childproofing Your Home for Poisons; Medication Safety Tips. HealthyChildren.org.
https://www.healthychildren.org/
[2] Wynn, P.M., Zou, K., Young, B., Majsak-Newman, G., Hawkins, A., Kay, B., Mhizha-Murira, J., & Kendrick, D. (2016). Prevention of childhood poisoning in the home: Overview of systematic reviews. International Journal of Injury Control and Safety Promotion, 23(1), 3-28.
[3] Huynh, A., Cairns, R., Brown, J.A., Lynch, A-M., Robinson, J., Wylie, C., Buckley, N.A., & Dawson, A.H. (2018). Patterns of poisoning exposure at different ages. Medical Journal of Australia, 209(2), 74-79.
[4] Australian Institute of Health and Welfare (AIHW). (2019). Trends in hospitalised injury, Australia 2007–08 to 2016–17.
[5] Schmertmann, M., Williamson, A., Black, D., & Wilson, L. (2013). Risk factors for unintentional poisoning in children aged 1–3 years. BMC Pediatrics, 13, 88.
[6] Rosenberg, M., Wood, L., Leeds, M., & Wicks, S. (2011). Parental perceptions and knowledge relating to childhood poisoning. Health Promotion Journal of Australia, 22(3), 217-222.
[7] Kendrick, D., Majsak-Newman, G., Benford, P., Coupland, C., Timblin, C., Hayes, M., Goodenough, T., Hawkins, A., & Reading, R. (2017). Poison prevention practices and medically attended poisoning in young children. Injury Prevention, 23(2), 93-101.
[8] Schwebel, D.C., Evans, W.D., Hoeffler, S.E., Marlenga, B.L., Nguyen, S.P., Jovanov, E., Meltzer, D.O., & Sheares, B.J. (2016). Unintentional child poisoning risk: A review of causal factors and prevention studies. Children’s Health Care, 46(2), 109-130.
[9] World Health Organization (WHO). Poison-control guidance and poisoning prevention materials.
https://www.who.int/
[10] Lee, K.A.Y.R., Harnett, J.E., & Cairns, R. (2019). Essential oil exposures in Australia. Medical Journal of Australia, 212(3), 132-133.
[11] Victorian Poisons Information Centre. (2018). Annual report 2018. Austin Health.
[12] Achana, F.A., Sutton, A.J., Kendrick, D., Wynn, P., Young, B., Jones, D.R., Hubbard, S.J., & Cooper, N.J. (2015). The effectiveness of interventions to promote poison prevention behaviours. PLoS One, 10(4), e0121122.
[13] World Health Organization (WHO). Lead poisoning and health fact sheet.
https://www.who.int/
[14] Quran, Surah An-Nisa 4:9
[15] Quran, Surah Al-Isra 17:36
[16] Quran, Surah Al-Ma’idah 5:2
[17] Sahih al-Bukhari 7138
[18] Sunan Ibn Majah 2340
[19] Sahih Muslim 2593